Red rashes… there are so many things that could look the same, and each child’s rash reacts a little differently. Even in the Bible many chapters in Leviticus was devoted to different skin lesions. There is only a small amount of treatments available…but oh so so soooooo many “boererate” and little ointments, potions and lotions that everybody swears worked for their child. Luckily eczema is one of the rashes we actually do have some answers for, so let me share what I do know:
What is Eczema?
Eczema (also called atopic dermatitis) is a chronic inflammatory skin disease that usually starts before the age of 5 years. It affects up to 1 in 5 children worldwide, and it seems as though it is becoming even more common in developed countries. You are not alone in your struggles!
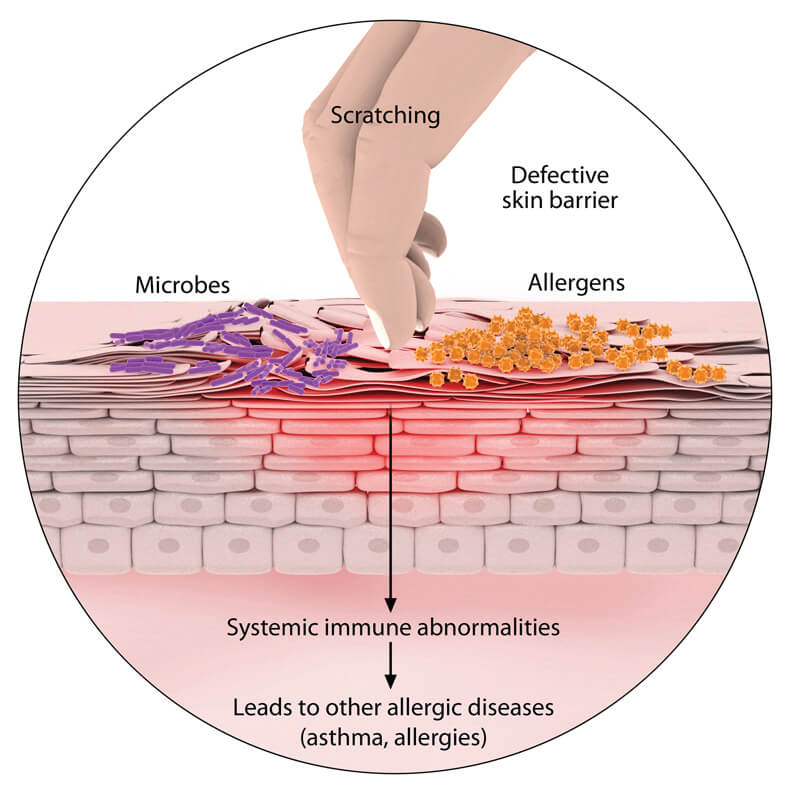
Genetics play a strong role so there is usually a family history that one or both parents have atopy (this means they are prone to food-allergies, eczema, allergic rhinitis and asthma). An abnormality in the outer barrier of the skin, the epidermis, leaves the skin vulnerable. Environmental irritants (such as grass, dust, heat, cold), allergens and microbes (such as bacteria and fungi) can now pass through, and the skin loses more water. Some children also have an abnormal immunological response to foreign proteins, worsening the inflammation of the skin. This cycle is a little like the debate about who comes first, the chicken or the egg. It is still unsure whether eczema starts “inside-out”, or “outside-in” and although specific food or aero-allergens can make it worse, it is not always the cause of eczema.
There is evidence that the microbiome on the skin (the “normal” bacteria and fungi that live on your skin in harmony) is disrupted in a child with eczema. This causes an overgrowth of bacteria (usually Staphylococcus Aureus) which could worsen the inflammation of the eczema. It is thus not a cause of eczema, but it can make it worse.
Symptoms:
Dry skin, intense itching, patches of red skin with small bumps and some flaking of the skin can be seen in children with eczema. There can also be some blistering and watery fluids leaking from the lesions, causing crusts on the skin. Itchiness is often worse at night. Scratching can worsen the inflammation and introduce infections. The skin can become thickened or darkened or even scarred from the constant inflammation and scratching.
Eczema usually start before one year of age, and the area of the body affected by the eczema can differ between children but can also change in the same child over time. Infants most commonly have patches on their arms and legs, their cheeks or scalp. Older children are more affected on their backs and the creases of their elbows and knees. Some children are only affected on their hands, or around their eyes or lips.
The eczema journey

Most children will outgrow their eczema by late childhood (80% clears up by 8years of age). If your child has a mild eczema and was diagnosed before 2yrs of age, the chances are good that your child will be eczema free soon.
However, if the eczema started before 2yrs of age, your child has a higher risk of developing other allergies and asthma. We call it the “allergic march”, meaning that if your child’s immune system is prone to over-react to foreign proteins encountered via the skin as a baby (resulting in eczema), it will probably overreact to food proteins encountered via the gut (resulting in food allergies), pollen proteins encountered via the nose (resulting in allergic rhinitis) and proteins encountered via the lungs (resulting in asthma) as your child grows. This does not mean that every child will develop all of the above, but we need to keep our eyes open for the signs and symptoms.
Children and adolescents with eczema can also develop ADHD, depression or anxiety disorders. This is thought to be caused by the lack of sleep due to night-time itching, the psychological stress of having a chronic disease as well as the effect of chronic inflammation on the developing brain.
There is also an association between Autism Spectrum Disorders and eczema. Children diagnosed with eczema before the age of 2 has a slightly higher risk to be diagnosed with autism later in life. This relationship is still being investigated, but it is thought that the different inflammatory markers (especially the cytokines) may play a role.
Eczema can thus affect all areas of your child’s life and they need close follow-up and care.
“Cast all your anxiety on him because he cares for you.” – 1 Peter 5:7
Making the Diagnosis:
Your GP can make the diagnosis by taking a good history and doing a quick examination of the skin. General practitioners should be able to treat mild cases, but if initial management does not work, it is better to follow up with a dermatologist and/or pediatrician to ensure good control of the disease.
Some diseases that could mimic eczema or that should be excluded are:
- Allergic or Irritant Contact dermatitis: This is when the skin reacts to a known allergen (eg a piece of fish touches your child’s hand he will get a rash only on his hand) or an irritant (eg your child wears new shoes and the rash is only visible where the shoe touched the foot.)
- Seborrheic dermatitis: mostly in infants. They develop a greasy red rash with scales on their scalp, eye brows and in their skin folds that is not itchy.
- Psoriasis: chronic auto-immune skin disease with red skin patches with a silvery scale. Rare in children
- Scabies: infection of the skin, very contagious, also very itchy. Usually there is a specific rash on the palms or in between the fingers.
- Certain drug reactions
- Primary immunodeficiency syndromes: here a lack of a certain part of the immune system may result in a rash on the skin.
I hope that you will feel more confident in understanding what eczema is and how it works and that this will empower you to tackle this journey with your child. Find a caregiver that you trust and will take alongside you on this journey. Treatment is available, and we will discuss it in next week’s post.
“He who has a why to live can bear almost any how.” – Friedrich Nietzsche
- Thorsteinsdottir S, Stokholm J, Thyssen JP, Nørgaard S, Thorsen J, Chawes BL, Bønnelykke K, Waage J, Bisgaard H; “Genetic, Clinical, and Environmental Factors Associated With Persistent Atopic Dermatitis in Childhood.”; JAMA Dermatol. 2019;155(1):50
- Kim JP, Chao LX, Simpson EL, Silverberg JI; “Persistence of atopic dermatitis (AD): A systematic review and meta-analysis.”; J Am Acad Dermatol. 2016;75(4):681. Epub 2016 Aug 17.
- Wan J, Mitra N, Hoffstad OJ, Gelfand JM, Yan AC, Margolis DJ; “Variations in risk of asthma and seasonal allergies between early- and late-onset pediatric atopic dermatitis: A cohort study”; J Am Acad Dermatol. 2017;77(4):634. Epub 2017 Aug 14.
- Yaghmaie P, Koudelka CW, Simpson EL;” Mental health comorbidity in patients with atopic dermatitis”; J Allergy Clin Immunol. 2013 Feb;131(2):428-33. Epub 2012 Dec 13.
- www.uptodate.com
- Thank you to the “National Jewish Health” site for the illustration.

One thought on “Eczema – Part 1”