Sniffles, Nunus, Snotties, Snottebellen… whatever you call it, we all know that when this fluid starts to run out of your child’s nose, or causes a complete blockage of their nostrils, we are in for a week or more of misery. I always say that if someone can find a use for this fluid, we would all be rich because there seems to be an unending supply in a toddler’s nose!



Today I want to look at the different causes and complications of a runny / blocked nose and then we will look at the different treatments in the next article.
In a healthy nose, the mucous secreted by the lining of the nose and sinuses, acts as a blanket to protect the lining against cold and dry air, and it is sticky enough to trap external particles, allergens and pathogens (viruses, bacteria, fungi).
What can cause a runny nose?
- Upper respiratory tract infections such as viral colds and flu or sinusitis.
- Allergic rhinitis – allergens such as pollen or grass triggers a release of histamine (part of an allergic reaction) which in turn causes itchiness, swelling of the nasal passages and an increase of mucous production.
- Teething – the inflammatory process around the erupting tooth can cause an excess of drooling and an increase of mucous in the nose.
- Inhaling strong spices, onions, perfumes or chemicals can act as irritants on the mucous membranes of the eyes and nose.
- If the mucous is draining from only one nostril, and it is foul smelling, there might be something stuck in that nostril! (Because toddlers love to push peas or small toys into little holes…)
Let us discuss upper respiratory tract infections in babies and toddlers:
Babies and toddlers have a high risk of upper respiratory tract infections due to their smaller airways, immature immune systems and the developmental need to put everything in their mouths! It is normal for children to have 6-8 upper respiratory tract infections per year. If they are in a crèche or school it may be 12-14 times a year because they are exposed to many more viruses and bacteria. Luckily they start to “outgrow” this phase by 5-6 years of age.
“Colds” (stuffy, runny nose, sneezing, scratchy throat,coughing, fever below 38.9’C) are mostly due to the rhinovirus (peaks in spring and autumn). The influenza virus (peaks in winter), respiratory syncitial virus (RSV), parainfluenza, adeno viruses, enterovirus and corona viruses are some of the other culprits (yes, different strains of the corona virus have been making trouble even before COVID 19 started).
Children get infected when they touch the secretions from an infected person and then touch their nose/mouth, or when they inhale the airborne virus that was coughed out by an infected person. Contrary to popular belief cold weather does not cause your child to become sick, but there are a few reasons why they tend to become sick during colder seasons: During the winter people are bundled up inside, windows are closed and the air is filled with a higher concentration of viruses and bacteria. The humidity drops causing dry nasal passages which makes it easier for viruses to enter the mucous membranes. Wearing an extra jersey will unfortunately not solve either of these problems. 😉
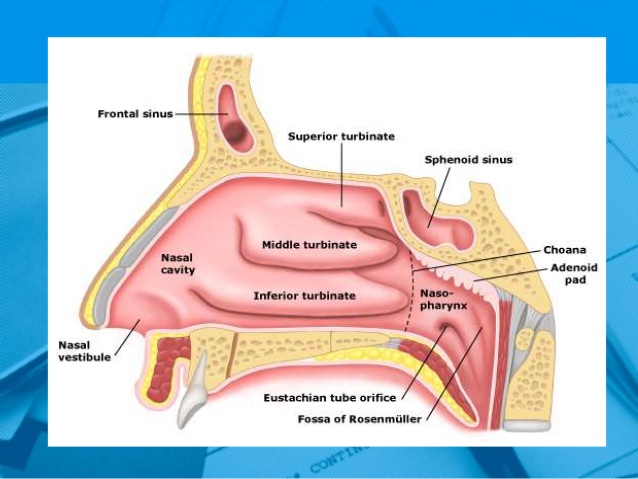
Once infected, the mucous membranes are irritated, which causes inflammation as the body tries to expel the virus by increasing the mucous secretions of the nasal passages and sinuses. There is also increased blood flow to the nasal passages, causing swelling and a blocked nose. The inflammatory “army” consists of different immune-cells rushing to the lining to fight off pathogens. As they die a heroic death, they are secreted into the mucous, causing the watery secretions to become white and then yellow. If a lot of the pathogens or other waste products are expelled in the mucous, it can even become green! It does not necessarily mean there is a bacterial infection; virus-waste products can also turn mucous green.
These excess secretions now drain via the nose and down the throat as a post-nasal drip which can irritate the throat and cause a cough that is worse at night when lying down. A post-nasal drip can also make children nauseous and cause bad breath.
“As the deer pants for streams of water, so my soul pants for you, my God” – Psalm 42:1
Most children will be sick for 3-5 days and then start to get better, but it is also normal for the symptoms to stick around for up to 14 days. In some children the virus itself can cause complications, and unfortunately a common cold causes the “perfect” conditions for bacteria to thrive, so some children develop secondary bacterial infections. (It is possible to have a primary viral infection of the sinuses, throat, tonsils and ears, so antibiotics are not always the answer for a red throat or tonsils!)
Possible complications (caused by the virus or by a bacterial infection):
- Sinusitis: when the sinuses are inflamed and infected it can cause prolonged symptoms (nasal discharge, post nasal drip and cough for more than 10 days), fever and facial pain.
- Tonsillitis: most children will have a bout of tonsillitis at least once in their lives. Some children have multiple episodes of bacterial tonsillitis leading to recurrent antibiotic use and eventually removal of the tonsils. In 2019 new research showed that some children with recurrent tonsillitis have a different type of immune cell in their tonsils that sabotage the formation of antibodies against Streptococcus A (the most common cause of bacterial tonsillitis) which makes them much more susceptible to infection with this bacteria. To prevent tonsillitis the child must not come into contact with the bacteria / the tonsils must be removed (this should be a last resort).
- Otitis media: The inner ear channels are connected to the throat via the Eustachian tube, making it easy for a post nasal drip to pool in the tube and for infection to spread to the inner ear. See my previous post about middle ear infections here.
- Breathing problems: babies prefer to breathe through their noses (to be able to drink and breathe at the same time) so if their little noses are blocked they are very uncomfortable and have to cry to keep their mouths open to breathe. Swelling of the small airways of the throat, lungs or of the vocal chords causes noisy breathing when breathing in (stridor) or out (wheezing). This might be due to croup or bronchiolitis (most common in babies up to 2 years of age) and it is important for a doctor to see them for further treatment .
- Pneumonia: rarely the infection spreads to the lung tissues either via the post-nasal drip that runs into the lungs (more commonly in babies with severe reflux) or via the bloodstream. This then becomes a “Lower Respiratory Tract Infection” and children will have fever and fast breathing. They may also show other signs of difficulty in breathing such as indrawing of the skin between the ribs, below the ribcage or above the breastbone (sternum) or flaring of the nostrils. In very ill babies their lips and fingers may turn blue (cyanosis) due to a lack of oxygen. These are all red flag signs that you need to see a doctor asap.
Now that you understand more of how an upper respiratory infection works, and where all the secretions come from, gather all your tissues until we can look at what we can do to prevent infections and how to treat it in the next article!
Resources:
- https://www.msdmanuals.com/home/children-s-health-issues/viral-infections-in-infants-and-children/overview-of-viral-respiratory-tract-infections-in-children
- Green RJ. Symptomatic treatment of upper respiratory tract infections in children. SA Fam Pract. 2006;48(4):38–42
- Paul IM, Beiler J, McMonagle A, Shaffer ML, Duda L, Berlin CM., Jr Effect of honey, dextromethorphan, and no treatment on nocturnal cough and sleep quality for coughing children and their parents. Arch Pediatr Adolesc Med. 2007;161(12):1140–1146
- https://www.healthline.com/health/postnasal-drip
- https://www.niaid.nih.gov/news-events/recurrent-tonsillitis
- Bakar MA, McKimm J, Haque SZ, Majumder MAA, Haque M; “Chronic tonsillitis and biofilms: a brief overview of treatment modalities”; J Inflamm Res; 2018: 11: 329-337
- https://www.nationwidechildrens.org/family-resources-education/700childrens/2018/01/humidifiers-for-respiratory-infections-are-they-helpful-or-harmful
- Wald E, Applegate KE et al; Clinical Practice Guideline for the Diagnosis and Management of Acute Bacterial Sinusitis in Children Aged 1 to 18 Years”; Pediatrics July 2013, 132 (1) e262-e280
- Zhang L, Mendoza-Sassi RA, Wainwright C, Klassen TP; “Is hypertonic saline solution via nebuliser effective and safe for infants with acute bronchiolitis?”; Cochrane review; 21 December 2017
